A patient of mine with long-standing AL amyloidosis was admitted to the hospital with congestive heart failure occurring in the setting of rapid atrial fibrillation ("AFib"). For non-medical folks, this means the top chambers of the heart (the atria) were beating extremely fast and irregularly, driving the bottom part of the heart (the ventricles) to do the same. This is not a kind thing of the atria to ask of the stiff, thick, amyloid-filled ventricles.
The situation was particularly difficult because of the patient's chronically low blood pressure. His typical BP of 90/50 was running even lower due to the abnormal heart rhythm. Some of the medications one might normally employ to control the Afib - like beta-blockers or calcium channel blockers - could not be used here because of the BP. I suggested to the medical residents that we try using digoxin, which would not be expected to lower the blood pressure. An hour later, the team called me back to let me know they had decided against that because the risk of digoxin toxicity was too high in this patient. I asked why they felt he was at risk for this, and the answer surprised me.
"His amyloidosis."
A search of PubMed using the search terms "digoxin" and "amyloidosis" yields only 8 references, at least as of the afternoon of May 18th, 2013. Of these, one of them was a case report of a person who was diagnosed with cardiac amyloidosis after developing fainting spells on digoxin. Another article describing two cases of familial transthyretin (ATTR) mentions in the abstract that such patients are prone to digoxin toxicity, but does not state that the patients in that report experienced this. I have thus far not been able to track don a copy of the actual article text. The other 6 references that came up were not relevant to my specific patient's case.
I tried another strategy and pulled up a review from cardiac amyloidosis guru Dr. Rodney Falk. Here is his commentary on the use of digoxin in AL amyloidosis patients:
"There is no role for digoxin in patients with cardiac amyloidosis who are in sinus rhythm. However, for patients with atrial fibrillation, cautious use of digoxin may aid in heart rate control although the risk of digoxin toxicity may be increased, possibly related to abnormal binding of the drug to amyloid fibrils."A reference for last statement not provided, so more digging was needed. Turned up the following additional references, not identified by original search:
A 1961 article from one of Michigan's own in the Annals of Internal Medicine which described two amyloidosis patients who seemed to have problems stemming from digitalis (a drug structurally related to digoxin, but with a longer half-life in the blood: 5-7 days, compared to 1.5-2 days). Pt #1 was a 58-yo farmer with jaundice and hypoalbuminemia (low serum protein levels) and atrial fibrillation who developed severe bradycardia (slow heart rate) of approximately 30 beats per minute after a 0.8 mg loading dose of digitalis followed a couple of days later by a 0.1 mg dose. Although it is not entirely clear from the text, it appears the patient had a liver biopsy proving he had systemic amyloidosis a few days before dying of liver failure. No information was provided regarding kidney function. On autopsy, multiple organs were confirmed to be infiltrated with amyloid, including the heart. Amyloid fibril typing was not performed. Pt #2, on the other hand, almost definitely had AL amyloidosis complicating a plasmacytoma. She was in sinus rhythm but had symptoms of congestive heart failure and exam findings suggesting cardiac tamponade (compressive fluid around the heart). She was treated with 1.3 grams of an older digitalis preparation (digitalis folia) over 60 hours. I cannot find a good reference with a dosage equivalency table to put this into current medical context. Also, again, no information on kidney function was provided. After dosing, the patient developed cardiac bigeminy (paired heart beats) with a rate of 70 beats per minute. The patient then developed severe hyperkalemia (high serum potassium levels - 8.3 mEq/L in this case, or about twice the normal level, after originally starting in the normal range). The patient suffered heart rhythm disturbances typical of this potassium level, and she died. On autopsy, the patient was found to have cardiac amyloidosis and a pericardial effusion (fluid around the heart) was confirmed. In 1961, serum digitalis levels were not obtainable.
A second article from A. Pomerance of London's Central Middlesex Hospital's Department of Morbid Anatomy and Histology was received at the British Heart Journal on Aug 17th, 1964, and was ultimately published in 1965. It turns out that at the exact same time, the Beatles were at work trying to get the tracks for Beatles for Sale! recorded and mixed. Busy time for the British. Pomerance's article is an autopsy series of 21 elderly patients with "senile amyloidosis." At the time, the composition of the fibrils had not been characterized; today we know that most if not all of these cases were likely ATTR (wild type) amyloid. The report is actually pretty fascinating from a historical standpoint, and it summarizes what was known at the time about systemic amyloidosis citing even older literature. As far as the cases, 3 of 21 patients were reported to have been "sensitive to digitalis" during hospital admissions prior to the terminal ones. No information about digitalis dosing, serum levels, or kidney function was provided. Two of the three patients had had prior myocardial infarctions.
So, 6 total cases of amyloidosis patients experiencing "digitalis sensitivity." One of the cases provides sufficient detail to justify this diagnosis. One (pt #2 from the 1961 Cassidy article) almost certainly did not experience digitalis sensitivity but died of hyperkalemia-induced arrhythmia in the setting of pre-existing cardiac tamponade. There is insufficient data on the other four patients (from Pomerance's report, and from the original PubMed search I did) to reach any conclusions one way or the other.
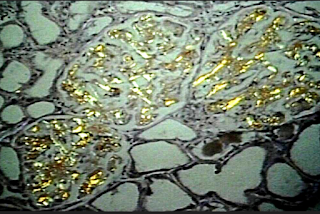
What about the last part of the cited text from the Falk article? The best support for this was a brief report by Dr A. Rubinow, Martha Skinner, and Alan Cohen from Boston University published in 1981. They describe a laboratory experiment in which they added digoxin to pellets of amyloid fibrils isolated from the spleens of three patients with amyloidosis, and also to samples of ground up tissues: normal human liver, normal human heart, and human heart affected by amyloidosis. They demonstrated that both pellets of pure amyloid fibrils or heart tissue from a patient with amyloidotic cardiomyopathy bound digoxin, whereas the control tissues (the ones without amyloid) did not.
 |
| Ref: http://circ.ahajournals.org/content/63/6/1285.long |
"Therapeutic judgement regarding the cautious administration of digoxin in patients with cardiac amyloidosis still rests on clinical grounds."
My conclusions? The same. Patients with amyloid cardiomyopathy are known to be at risk for potentially fatal arrhythmias - its what accounts for the dismal outcomes seen in patients with cardiac stage 3 AL amyloidosis. It is also clear that patients with structural heart injury from any cause may be at risk for digoxin-induced arrhythmias. So caution is warranted. A critical review of the literature, however, does not make the case that digoxin can never be used in patients with systemic amyloidosis.